2006 orvieto, giornate cardoilogiche orvietane. il trattamento non farmacologico dello scompenso...
-
Upload
centro-diagnostico-nardi -
Category
Health & Medicine
-
view
53 -
download
2
Transcript of 2006 orvieto, giornate cardoilogiche orvietane. il trattamento non farmacologico dello scompenso...

Giornate Cardiologiche OrvietaneGiornate Cardiologiche OrvietaneIl trattamento non farmacologico dello Il trattamento non farmacologico dello
SCOMPENSO CARDIACOSCOMPENSO CARDIACOStefano Nardi, MD, PhD
AZIENDA OSPEDALIERA SANTA MARIA TERNI AZIENDA OSPEDALIERA SANTA MARIA TERNI DIPARTIMENTO CARDIOTORACOVASCOLARE DIPARTIMENTO CARDIOTORACOVASCOLARE STRUTTURA COMPLESSA DI CARDIOLOGIASTRUTTURA COMPLESSA DI CARDIOLOGIA
STRUTTURA SEMPLICE DI ARITMOLOGIA STRUTTURA SEMPLICE DI ARITMOLOGIA LABORATORIO DI ELETTROFISIOLOGIA ED ELETTROSTIMOLAZIONE LABORATORIO DI ELETTROFISIOLOGIA ED ELETTROSTIMOLAZIONE

CHFCHF: non pharmacological approach: non pharmacological approach

Reduced Mortality in HFACE-I & Beta Blockade
Reduce Mortality
11.5%
15.6%12.4%
7.8%
0%4%8%
12%16%
SOLVD-T MERIT-HF+ CIBIS II
1 Ye
ar M
orta
lity
Placebo Treatment
CHFCHF: non pharmacological approach: non pharmacological approach
Digossina, Diuretici, Idralazina ACE-I
ß-blocker and ACE-I
SOLVD CONCENSUS da -16 a -31% CIBIS II
COPERNICUS - 35%
Mortalità
Mortality Mortality
too Hightoo High

Mortalità ad 1 annoITALIAN NETWORK CHF
4,1 %4,1 %
11,7 %11,7 %
24,8 %24,8 %
36,7 %36,7 %
15,1 %15,1 %
(%)(%)
NYHA I1
NYHA II2,14
[1,33-3,44]
NYHA III3,77
[2,32-6,12]
NYHA IV5,54
[3,23-9,48]
TotaleRischio Relativo
• 600.000 CHF pts• 87.000 morti / anno• Mortalità a 5 anni >70%• 44% CHF re-hospitalization
a 6 mesi dal primo evento• % della spesa sanitaria per
CHF: 1,5 - 2% • CHF prima causa di
ospedalizzazione nella popolazione > 65 anni di età
• CHF prima patologia per durata della degenza ospedaliera
1 Framingham Heart Study (‘48 – ‘88) in Atlas of Heart Diseases.2 AHA. Heart Disease and Stroke Statistics—’03 Update.
CHF Patients Survival Results1CHF Patients Survival Results1
CHFCHF: non pharmacological approach: non pharmacological approach

a Vicious Cycle
Abnormal RV-LV sequence
Mitral Regurgitation
Segmental Dyskinesia
Dysynchronous Contraction
Abnormal LV activation sequence
↑ Neurohormones
↓ LVEF
Dissynchrony RV/LV
filling flow
CHFCHF: non pharmacological approach: non pharmacological approach

Burkhoff D, Am J Phys ‘87
Different Pacing-site in CANINE model
What does it mean What does it mean Asynchronus activation ? Asynchronus activation ?
CHFCHF: non pharmacological approach: non pharmacological approach

Spragg DD, Circulation ’03
Regional Alterations of Protein Expression in CHF dogs
CHFCHF: non pharmacological approach: non pharmacological approach

SinusSinusnodenode
AVAVnodenode
BundleBundlebranch orbranch or
diffuse blockdiffuse block
Delayed conductionDelayed conduction
• Abnormal RV-LV sequence• Abnormal LV activation
sequence• Segmentary dyskinesia• Aggravation of mitral
regurgitation• Disynchrony of RV and LV
filling flows
Dyssynchrony Ventricular ContractionDyssynchrony Ventricular Contraction
What is abnormal in the HF pts?What is abnormal in the HF pts?• Delayed AV sequence• Mitral regurgitation• Decreased filling time
CHFCHF: non pharmacological approach: non pharmacological approach

What does it means DYSSYNCHRONYSM ?
0
5
10
15
20
25
301 Year-Mortality
Total Sudden Death
LBBBNo LBBB
Study pop
11.9
16.1
10.5
5.5 4.97.3
p<0.001
p<0.001
60%
70%
80%
90%
100%
0 60 120 180 240 300 360Days in Trial
Cu
mu
lati
ve S
urv
ival
QRS Duration (msec)
<9090-120
120-170170-220
>220
Adapted from Gottipaty et al. JACC 1999; 33(2):145A (abstract 847-4)
INCHF
• VEST study analysis• NYHA Class II – IV pz
CHFCHF: non pharmacological approach: non pharmacological approach

Di Donato M, Circulation ‘04
Which is the relationship between Dysshynchronysm and QRS duration ?
60%
70%
80%
90%
100%
0 60 120 180 240 300 360Days in Trial
Cu
mu
lati
ve
Su
rv
iva
l
Ole-A. Breithardt, MD
ALTERED WORK-LOAD
CHFCHF: non pharmacological approach: non pharmacological approach

• Radionuclide • MRI • ECHO-cardiography
Which technique for Patients selection ??
INTER-VCD (CARE HF) Conventional Echo-Doppler (Q-efflux Ao –Q-efflux Po >40 ms)
INTRA-VCD M-mode (validate only in QRS wide) PW-TDI Strain Rate Echo 3D
CHFCHF: non pharmacological approach: non pharmacological approach

• Optimizes AV contraction sequence
• Reduces pre-systolic mitral regurgitation
• Improves atrial preloading of the ventricle
• Increases filling time
Mechanism IMechanism IAtrio-Ventricular SynchronyAtrio-Ventricular Synchrony
Rationale for CRTRationale for CRT What does pacing changeWhat does pacing change??
CHFCHF: non pharmacological approach: non pharmacological approach

• Optimizes ventricular activation• Increases pumping effectiveness• Reduces regional wall stress (WMSI)• Decreases mitral regurgitation• Resynchronizes ventricular filling flows• Decreases filling pressures
Mechanism IIMechanism IIVentricular CoordinationVentricular Coordination
Rationale for CRTRationale for CRT What does pacing changeWhat does pacing change??
CHFCHF: non pharmacological approach: non pharmacological approach

OAVD Restores AV Synchrony
PP RR
INTRINSICINTRINSICAorticAortic
pressurepressure
LVLVpressurepressure
PPPP
PeakPeakatrial systoleatrial systole
Start ofStart ofLV systoleLV systole
DiastolicMitral
Regurgitation
MaximumEffective Preload
PP VV
PACEDPACEDPPPP
SynchronizedSynchronizedLV and atrialLV and atrial
systolessystoles
Auricchio, PACE `98
CHFCHF: non pharmacological approach: non pharmacological approach

Kass et al, Kass et al, Circulation 99Circulation 99
IntrinsicIntrinsicPacedPaced
00 100100 200200 30030000
4040
8080
120120RV SeptumRV Septum
00 100100 200200 30030000
4040
8080
120120BiventricularBiventricular
00 100100 200200 30030000
4040
8080
120120RV ApexRV Apex
00 100100 200200 30030000
4040
8080
120120LV FreewallLV Freewall
LV Volume LV Volume (mL)(mL)
LV P
ress
ure
LV P
ress
ure
(mm
Hg)
(mm
Hg)
LV P
ress
ure
LV P
ress
ure
(mm
Hg)
(mm
Hg)
LV Volume LV Volume (mL)(mL)
Acute studiesCHFCHF: non pharmacological approach: non pharmacological approach

Cumulative Enrollment in C.R. Cumulative Enrollment in C.R. Randomized TrialsRandomized Trials
0
1000
2000
3000
4000
1999 2001 2003 2005
Result s Present ed
Cum
ulat
ive
Pati
ents
PATH CHF
MUSTIC SRMUSTIC AF
MIRACLE
CONTAK CD
MIRACLE ICD
PATH CHF II
COMPANION
MIRACLE ICD II
CARE HF
DOUG SMITHDOUG SMITH
CHFCHF: non pharmacological approach: non pharmacological approach

Auricchio et al., NASPE ‘99
PATH-CHF: Inclusion Criteria (42 pts)
• Dilated cardiomyopathy of any etiology• NYHA Class III (> 6 months) or NYHA IV• Optimal individual drug therapy • QRS duration >120 msec • PR Interval >150 msec• Sinus rate > 55 bpm• No conventional pacemaker indication
PATH CHF
CHFCHF: non pharmacological approach: non pharmacological approach

325
350
375
400
425
450
475
pre-implantn=20
4 weeksn=20
8 weeksn=20
12 weeksn=20
6 monthsn=20
12 monthsn=20
Meter
s
Long Term Benefit PATH CHF
Auricchio et al., NASPE ‘99
0
10
20
30
40
50
60
pre-implantn=20
4 weeksn=20
8 weeksn=20
12 weeksn=20
6 monthsn=20
8 monthsn=20
10 monthsn=20
12 monthsn=20
Minnes
ota Sc
ore
Quality of Life6 - MWT
CHFCHF: non pharmacological approach: non pharmacological approach

Long Term Benefit: Peak Oxygen Uptake
0.9
1
1.1
1.2
1.3
1.4
0 1 2 3 4 5 6 7 8 9 101112
Months
Peak
VO2
(l/min)
PATH CHF
Auricchio et al., NASPE ‘99
0
10
20
30
40
days
of
hosp
italiz
ation
1 Year1 YearPre-ImplantPre-Implant
1 Year1 YearPost-ImplantPost-Implant
P P == .003 .003
CHFCHF: non pharmacological approach: non pharmacological approach

MIRACLE Inclusion Criteria (571 pts)
• Moderate or severe HF (NYHA III-IV)• Stable optimal HF medical therapy regimen
for >1month - Diuretics (93-94%) - ACE-I or ARB (90-93%) if tollerated - β-blocker (55-62%) at stable regimen for>3 months
• QRS duration ≥150 msec • LVEF ≤35% or LVEDD ≥55mm (echo measure)• Sinus rate > 55 bpm • 6 MWT <450m
Abraham WT, Fisher WG, Smith AL, et al. N Engl J Med 2002;346:1845-1853
CHFCHF: non pharmacological approach: non pharmacological approach

Benefits Sustained Through 2 yr: MIRACLE Study Program
0100200300400500
Mean 6-MWT(m)
1
2
3
4
020406080
100
6 (N=1124) 12 (N=693) 18 (N=320) 24 (N=68)
Months of Active CRT
Mean NYHAFunctional Class
Mean QoL Score Improvement ↓
Baseline Follow-up
PairedDataDisplayed
P<0.001 P<0.001 P<0.001 P=0.01
P<0.001 P<0.001 P<0.001 P<0.001
P<0.001 P<0.001 P<0.001 P<0.001
Source: Abraham, WT et al. AHA 2003
CHFCHF: non pharmacological approach: non pharmacological approach

Change in MR Jet AreaChange in MR Jet Area
-4-4-3-3-2-2-1-10011
ControlControl(n=118)(n=118)
CRTCRT(n=116)(n=116)
cmcm22
P<0.001P<0.001 P=0.009P=0.009
Change in LVEDDChange in LVEDD
-6-6
-4-4
-2-2
00
22
ControlControl(n=118)(n=118)
CRTCRT(n=116)(n=116)
mmmm P<0.001P<0.001
Absolute Change in LVEFAbsolute Change in LVEF
-2-2
00
22
44
66
88
ControlControl(n=146)(n=146)
CRTCRT(n=155)(n=155)
%%
Baseline (mm)Baseline (mm)69 ± 10
70 ± 10Baseline (cmBaseline (cm 2)
7.2 ± 4.9
7.6 ± 6.4Baseline (%)Baseline (%)
22 ± 6
22 ± 6
Paired median change from baseline at 6 months
Cardiac Function and StructureMIRACLE
CHFCHF: non pharmacological approach: non pharmacological approach

Effects on Cardiac Function and Oxidative Stress
0,14
0,16
0,18
0,20
0,22
0,24
500 600 700 800 900
dP/ dt max ( mm/ Hg/ s)
MVO
2/HR
(Rel
ative
Unit
s) Dobutamin
LV Pacing
P< 0.05
Nelson et al. Circulation 2000
Myocardial Oxidative Metabolism
0
0,02
0,04
0,06
LV RV
k mon
o(min
-1)
p=0.86
p=0.62
n=8
Myocardial Efficiency Work Metabolic Index
0
2
4
6
8
10
12
mm
HG
·L·m
-2
Baseline CRT
p =0.024
Ukkonen et al. Circulation 2003
n=7
MIRACLE
CHFCHF: non pharmacological approach: non pharmacological approach

Mortality/Morbidity from Published Randomized, Controlled Trials
Risk reduction with CRT
Study (n random.) FU
Mor-tality & Hosp.
Mortal. & HF Hosp.
Mor-tality
HF Mort.
HF Hosp.
MIRACLE (n=453)
6 Mo NR 39%* 27% NR 50%*
MIRACLE ICD (n=369)
6 Mo 2% 0% 0% NR NR
Contak CD (n=490)
3-6 Mo NR NR 30% NR 18%
Meta-analysis (n=1634)
3-6 Mo NR NR 23% 51%* 29%*
* P < 0.05
CHFCHF: non pharmacological approach: non pharmacological approach

RandomizeRandomize1:2:21:2:2
• Optimal Optimal Pharmacologic Pharmacologic Therapy (OPT)Therapy (OPT)
• OPTOPT
• BV pacingBV pacing +
• OPTOPT
• BV pacingBV pacing
• DefibrillationDefibrillation
+
CoComparison of mparison of MMedical Therapy, edical Therapy, PPacing acing anand d DefibrillatDefibrillationion in Chronic Heart Failure in Chronic Heart Failure ((COMPANIONCOMPANION))
CHFCHF: non pharmacological approach: non pharmacological approach

COMPANION CARE - HF
Cleland J. G.F, NEJM ‘05Bristow, NEJM ‘04
CHFCHF: non pharmacological approach: non pharmacological approach

• Reduced LVEF remains the single most important risk factor for overall mortality and SCD.1
• Increased risk is measurable at EF above 30%, but an EF ≤30% is the single most powerful independent predictor for SCD.2
1Prior SG, Aliot E, Blonstrom-Lundqvist C, et al. Task Force on Sudden Cardiac Death of the European Society of Cardiology. Eur Heart J, Vol. 22; 16; August 2001.2 Myerburg RJ, Castellanos A. Cardiac Arrest and Sudden Cardiac Death, in Braunwald E, Zipes DP, Libby P, Heart Disease, A textbook of Cardiovascular Medicine. 6th ed. 2001. W.B. Saunders, Co., p. 895.
Relationship of SCD Relationship of SCD and LV Dysfunctionand LV Dysfunction
CHFCHF: non pharmacological approach: non pharmacological approach

Several RANDOMIZED studies have demonstrated that ICD reduce MORTALITY (~30-50%), both in primary and in secondary prevention
CHFCHF: non pharmacological approach: non pharmacological approach

• 126 pts underwent CRT • If criteria for ICD
(US guidelines, including MADIT) CRT-D
• If no, CRT-P
CRT-D vs CRT-P in Severe LV dysf. Ermis et al. JCE, ‘04
Miglioramento del 41% (p =0,01)
I pazienti che non presentano rischi noti di Morte Improvvisa li sviluppano col passare del tempo …ecco perché necessitano di un ICD di back-up
CHFCHF: non pharmacological approach: non pharmacological approach

Mortalità totale
Frazione di eiezione
Morte per causa aritmica
Diss. E-M ElettricaInfettiva
NeoplasticaNeurologica
Ecc. All’aumentare della LVEF si riduce la mortalità per CHF ma aumenta quella per causa aritmica
Challenges in electrical management of CHF
NYHA II
Other24%
CHF12%
Sudden death64%
N=103
NYHA III
Sudden death59%
CHF26%
Other15%
N=232
NYHA IV
Sudden death33%
CHF56%
Other11%
N=27 MERIT-HF
CHFCHF: non pharmacological approach: non pharmacological approach

ACE-I & Beta Blockade Reduce Mortality
11,5%
15,6%12,4%
7,8%
0%4%8%
12%16%
SOLVD-T MERIT-HF+ CIBIS II
1 Ye
ar M
orta
lity
Placebo Treatment
Further Reduction with CRT + ICD
for Higher Risk PatientsHF
Mortality
SuddenCardiac Death
CRT
ICD
Weight of Evidence: CRT
CHFCHF: non pharmacological approach: non pharmacological approach

Digossina, Diuretici, Idralazina ACE-I
ß-blocker and ACE-I ß-blocker,
ACE-I and CRT-D
COMPANION - 36%
SOLVD CONCENSUS da -16 a -31% CIBIS II
COPERNICUS - 35%
Mortalità
CONCLUSIONSCONCLUSIONS
CHFCHF: non pharmacological approach: non pharmacological approach

D’Ascia C, Eu Heart J ‘06
CRT
Baseline 1wk 1mo 3mo off-immed off-1wk off-4wk
100
125
150
175
200
225
**
*
*
†
* *
*
†
Left
ven
tric
ular
vol
ume
(mL) *
VO2
(ml/
min
/mVO
2 (m
l/m
in/m
22 ))
DODO22 (ml/min/m (ml/min/m22))
Critical DOCritical DO2 2
DISOXIADISOXIA
Critical VOCritical VO22
NormalNormal
ReverseRemodelling
TNF-alpha expressionApoptosisFibrosis
CHFCHF: non pharmacological approach: non pharmacological approach

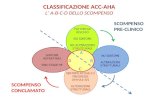
2002 Classe IIa: Symptomatic pts, Class NYHA III or IV, DCM (hydiopatic or ischemic) prolonged QRS interval (≥ 130 ms), LVEDD≥ 55 mm, LVEF ≤ 35%.
News 2005Classe I:Symptomatic pts, Class NYHAIII, Synus Rhythm, OMT forCHF, Dyssynchrony
(Level of Evidence A)
Aggiornamento delle linee guida ACC/AHA (2002 2005) →
Terapia CRT
CHFCHF: non pharmacological approach: non pharmacological approach

ESC 2005 Classe IIa: Symptomatic pts in NYHA Class III or IV in OMT for CHF, Dyssinchrony and reduced LVEF
ACC/AHA 2005Classe I:Symptomatic pts, Class NYHAIII, Synus Rhythm, OMT forCHF, Dyssynchrony
(Level of Evidence A)
Confronto tra LINEE GUIDA ESC e ACC/AHA (2005)
Terapia CRT
CRT for improve symptoms and CHF-H (Level of Evidence A)
CRT for improve risk of death (Level of Evidence B)
CHFCHF: non pharmacological approach: non pharmacological approach

CLASS I SR, LVEF ≤ 35%, QRS > 120ms, NYHA III-IV, OMT
CLASS II
Atiral Fibrillation LVEF ≤ 35%, QRS > 120ms, NYHA III-IV in OMT LVEF ≤ 35%, QRS ≤ 120 ms, NYHA III-IV, OMT Dysshynchronism (Echo), SR, LVEF ≤ 35%, QRS > 120msSymptomatic NYHA class II, PM or ICD indication (in primary prevention) Chronic RVA pacing, LVEF ≤ 35%, NYHA III-IV, OMT, Severe Dyssynchronism (Up-grading),
LINEE GUIDA AIAC 2006CRT
CHFCHF: non pharmacological approach: non pharmacological approach

High anatomic of CS system
Optimization of CRT
(n° vene, presenza di valvole, angolature,
tortuosità ecc.)
CHFCHF: non pharmacological approach: non pharmacological approach

• Reduction of responsivity in ischemic disease (SCAR, Non contractile segment etc) (Gasparini M, PACE ’03)
• In Ischemic DCM the asynchronysm can interest each LV wall, whereas CRT is more efficacy in lateral or postero-lateral wall (Yu CM, Circulation ‘04)
• Pacing not efficacy• Comorbidity• Severe CHF or hemodinamic
instability
Why are the Non-Responders ?CHFCHF: non pharmacological approach: non pharmacological approach

• No MR (Reuter S et a. Am J Cardiol ‘02) or severe MR (Achilli A, Italian Heart J ‘04)
• Elevated LVEDV and LVESV (Bax JJ, JACC ‘04)
• Permanent AFib - controverso: ablazione NAV? Speranza di recupero RS con riduz. IM e reverse LV remodeling?
• Class NYHA IV
Why are the Non-Responders ?CHFCHF: non pharmacological approach: non pharmacological approach

CHF Population
6.5 Mio
NYHA III + IV (30 - 35%)
1.95 Mio
Wide QRS (10 - 30%)
Resynchronization Rx Target Population:195’000
650’000
Incidence = 580’000 (9.0%)Mortality = 300’000 (4.6%)
CHF Population in EuropeCHF Population in EuropeCHFCHF: non pharmacological approach: non pharmacological approach

Relative Cost of CRTCost per pat ient
$0$20$40$60
CRT+ I CD
CRT
Hip/ knee replace
PTCA
CABG
Dialysis
$ t housands
Total Annual Expenditures
$0 $5 $10 $15 $20
$ BillionsDoug Smith:
Doug Smith:
CONCLUSIONSCONCLUSIONS
CHFCHF: non pharmacological approach: non pharmacological approach

0
5000
10000
15000
Baseline Post-implant
Intensive careCardiologyOthers
Patient Cost Baseline: 12,784 Euro Patient Cost (Implant included): 12,362 EuroPatient Cost Post-implant: 1,680 Euro
Hospital costs per patient
Cost EffectivenessAnalysis of Biventricular Pacing in HF
Curnis A 2001
CONCLUSIONSCONCLUSIONSCHFCHF: non pharmacological approach: non pharmacological approach

Creating Realistic patients expectations
• Approximately two-third of patients should experience improvement, but some patients may not experience immediate improvement
• Have patients set their own goals of what they would like to do following CRT: Grocery shopping, Decreasing Lasix dose, Walking to the mailbox without stopping, Lying flat to sleep
CHFCHF: non pharmacological approach: non pharmacological approach

Necessari ulteriori studi con “follow-up” a più lungo termine per capire il giusto
“LINK” esistente tra efficacia in ACUTO, mantenimento del risultato in cronico e
CONSEGUIMENTO DEGLI “END POINT”
Perfezionare le conoscenze sui meccanismi della CHF
Migliorare la tecnologia, rendere le procedure sempre più fattibili
minimizzando i rischi
CHFCHF: non pharmacological approach: non pharmacological approach

GRAZIE PER LA GRAZIE PER LA CORTESECORTESE
ATTENZIONEATTENZIONE
CHFCHF: non pharmacological approach: non pharmacological approach

• Have patients set their own goals of what they would like to do following CRT: Grocery shopping, Decreasing Lasix dose Walking to the mailbox without stopping, Lying flat to sleep
• Encourage them to be part of the group that responds to their therapy
Creating Realistic expectations
Cardiac Resynchronization TherapyCardiac Resynchronization Therapy

DEPOSITODEPOSITO

InSync Italian Registry
QRS duration (msec) 172+32Ejection fraction (%) 25+7LV end Diast. Diameter (mm) 71+9NYHA functional class 3,15+0,616 min walking test (m) 269+142Chronic Atrial Fibrillation 17,4%
190 patients M= 82,8%; Age= 68+ 8ETIOLOGY: Ischemic 46,6%; Idiopatic 37,9%; Other 15,5%
InSyncItalianRegistry
Cardiac Resynchronization TherapyCardiac Resynchronization Therapy

InSyncItalianRegistry
M. Zardini et al, Eur Hear 2000
LVEF %
0
10
20
30
40
BASELINE FOLLOW-UP
%
6m HWT
0
100
200
300
400
500
BASELINE FOLLOW-UP
m
NYHA class
0
1
2
3
4
BASELINE FOLLOW-UP
QOL Score
0
10
20
30
40
50
60
70
80
BASELINE FOLLOW-UP
p < .0001
p < .0001 p < .0001
p < .0001
Clinical Outcome
Cardiac Resynchronization TherapyCardiac Resynchronization Therapy

Results Active pacing
Inactivepacing
p
6-min w (m) 399 ± 100 326 ± 134 .0001QOL score 29.6 ± 21.3 43.2 ± 22.8 .0002VO2 (ml/min/Kg) 16.2 ± 4.7 15 ± 4.9 0.02
S.Cazeau et al NEJM 2001;344:873-80S.Cazeau et al NEJM 2001;344:873-80
MUSTIC Results (67 pts)
Cardiac Resynchronization TherapyCardiac Resynchronization Therapy

VO2
(ml/
min
/mVO
2 (m
l/m
in/m
22 ))
DODO22 (ml/min/m (ml/min/m22))
OO22ERER
Critical DOCritical DO2 2
DISOXIADISOXIA
Critical VOCritical VO22
DODO22 = = QQC C X CaX CaOO22
VOVO22 = = DODO2 2 X X OO22ERER
NormalNormal
DODO22 = =QQC C x (1,34 xx (1,34 x Hb x Sa Hb x SaOO22) x 10) x 10
Cardiac Resynchronization TherapyCardiac Resynchronization Therapy

QOL & Functional Capacity 6 Months in Moderate to Severe HF
-20-15-10-50
P<0.001 P=0.02 P=0.017P<0.001
QoL Score(MLWHF)
Avg. Change
0%20%40%60%80%
MIRACLE MUSTIC SR MIRACLE ICD Contak CD
P<0.001 P=0.006P=0.007
Data sources:MIRACLE: Circulation 2003;107:1985-90 MUSTIC SR: NEJM 2001;344:873-80MIRACLE ICD:JAMA 2003;289:2685-94 Contak CD: JACC 2003;2003;42:1454-59
Control CRT
NYHA ClassProportionChanging 1
or more Classes
Improve. ↓
Not Reported
Cardiac Resynchronization TherapyCardiac Resynchronization Therapy

Exercise Capacity 6 Months in Moderate to Severe HF
-20
0
20
40
60 P<0.001 P=0.36 P=0.029P<0.001
6 Min WalkAvg. Change
(m)
000
1
2
3
MIRACLE MUSTIC SR MIRACLE ICD Contak CD
P<0.001
P=0.029
P=0.04P=0.003
Data sources:MIRACLE: Circulation 2003;107:1985-90 MUSTIC SR: NEJM 2001;344:873-80MIRACLE ICD:JAMA 2003;289:2685-94 Contak CD: JACC 2003;2003;42:1454-59
Control CRT
Peak VO2
Avg. Change (mL/kg/min)
Cardiac Resynchronization TherapyCardiac Resynchronization Therapy

Effect on LV Structure Effect on LV Structure 6 Months in Moderate to Severe HF
-40
-20
0
P<0.001P=0.06
LVEDVAvg. Change
(mL)
-6-4-202
MIRACLE MIRACLE ICD Contak CD
P<0.05 P=0.81 P=0.001
Control CRT
LVEDDAvg. Change
(mm)
NOT REPORTED
Data sources: MIRACLE: Circulation 2003MIRACLE ICD:JAMA 2003CONTAK CD: J Am Coll Cardiol 2003
Cardiac Resynchronization TherapyCardiac Resynchronization Therapy

0
2
4
6
P<0.001P=0.12
P=0.029
LVEFAvg. Change(Absolute %)
-3-2-10
MIRACLE MIRACLE ICD Contak CDP<0.001
P=0.58
Data sources: MIRACLE: Circulation 2003MIRACLE ICD:JAMA 2003CONTAK CD: J Am Coll Cardiol 2003 Control CRT
MR Jet AreaAvg. Change
(cm2)
Not Reported
Effect on LV Function Effect on LV Function 6 Months in Moderate to Severe HF
Cardiac Resynchronization TherapyCardiac Resynchronization Therapy

CRT Does Not Promote Ventricular Arrhythmias
• Analyzed 1,044 patients with ICDs from 2 trials:– CONTAK CD– MIRACLE ICD
• Odds ratio (CI):0.92 (0.67 – 1.27)
Patients with VT or VF during Follow-up
17,2%18,4%
No CRT CRT
Prop
orti
on
Bradley DJ, et al. JAMA 2003
Cardiac Resynchronization TherapyCardiac Resynchronization Therapy

Left Ventricular End Systolic Diameter
200
250
300
350
400cm3
Base 6 Mo
P=0.01
CRT Promotes Reverse Remodeling in Class II CHF
Left Ventricular End Diastolic Diameter
200
250
300
350
400cm3
Base 6 Mo
P=0.04
Left Ventricular Ejection Fraction
20
22
24
26
28
30%
Base 6 Mo
P=0.02
• Control (n=85) ♦ CRT (n=69)
MIRACLE ICD II
Cardiac Resynchronization TherapyCardiac Resynchronization Therapy

• Radionuclidi • RMN • ECOcardiografia
Patients selectionCardiac Resynchronization TherapyCardiac Resynchronization Therapy
INTER-VCD Eco-Doppler convenzionale (Q-efflusso Ao –Q-efflusso Po >40 msec)
INTRA-VCD Eco M-mode (validate only in QRS wide) PW-TDI Strain Rate Echo 3D
Quando isolata, BASSO VALORE PREDITTIVO

DCM - Ischemic
Advanced age
NYHA Class IV
PeAF No MR
Maggiori LVEDV LVESV
Cardiac Resynchronization TherapyCardiac Resynchronization TherapyWhy are the Non-Responders ?

Cardiac Resynchronization TherapyCardiac Resynchronization TherapyRelated Risks
Complicat ions ( 1)
4,8
3,7
1,5
1,0
1,8
0,3
10,6
10,0
2,3
2,4
1,7
0,3
0 5 10 15
Unsucess. Implant
LV Lead
Coronary Sinus
Infection
30 day mortality
Procedure death
Percent of Pat ient s
MIRACLE+CONTAKCD+MIRACLE ICD
InSync III/Attain4193
Reduced Procedure Time w it h I ncreased Exper ience (2)
60
120
180
240
300
Up t o f ir st5
Next 6 t o10
Next 11more
Cent er-based exper ienceIm
plan
t Ti
me
(min
utes
) P < 0.001
Study Period AttemptsPrimary LV Lead
MIRACLE 11/98 – 12/00 591 Attain 2187
Contak CD 2/98 – 12/00 517 EasyTrak
MIRACLE ICD 10/99 – 8/01 636 Attain 4189
InSync III 11/00 – 6/02 334 Attain 4193
1. Greenberg, et al. PACE 2003;26(4p2): 952 (Abstract 93)
2. Unpublished data. Medtronic. Inc.

Relazione di Frank-Starling
P intraventric. (mmHg)
= sviluppo di forza
50
100
150
200
250
50 100 150 200 250
Volume ventricolare sinistro (ml)= lunghezza iniziale della fibra miocardica
sistole
diastole
Definizione: entro limiti fisiologici, tanto più il cuore si riempie durante la diastole, tanto maggiore sarà la quantità di sangue pompata in aorta in sistole
Cardiac Resynchronization TherapyCardiac Resynchronization Therapy

1 Framingham Heart Study (1948 – 1988) in Atlas of Heart Diseases.2 American Heart Association. Heart Disease and Stroke Statistics—2003 Update.
CHF Patients Survival ResultsCHF Patients Survival Results11
1009080
70
605040
3020100
Prob
abili
ty o
f su
rviv
al, %
Men (Men (n n = 237)= 237)Women (Women (nn = 230) = 230)
Time after CHF diagnosis, years0 2 4 6 8 10
80% of men and 70% of women who have CHF will die within 8
years.2
80% of men and 70% of women who have CHF will die within 8
years.2
Cardiac Resynchronization TherapyCardiac Resynchronization Therapy

NYHA CLASS
Ann
ual s
urvi
val (
%)
Hos
pita
lizat
ions
/ y
ear
100
75
50
25
0I II III IV
1
10Survival
Hospitalization
.1
Hospitalization / NYHA-classCardiac Resynchronization TherapyCardiac Resynchronization Therapy

Volume Volume OverloadOverload
Pressure Pressure OverloadOverload
Loss of Loss of MyocardiumMyocardium
Impaired Impaired ContractilityContractility
LV Systolic DysfunctionEF < 35%
↓↓ Cardiac Cardiac OutputOutput
Hypoperfusion Hypoperfusion
↑↑ End Systolic Volume End Systolic Volume
↑↑ End Diastolic Volume End Diastolic Volume
Pulmonary Congestion Pulmonary Congestion
LV Systolic DysfunctionCardiac Resynchronization TherapyCardiac Resynchronization Therapy

Proposed Mechanisms of Benefit
IntraventricularSynchrony
AtrioventricularSynchrony
InterventricularSynchrony
↑ dP/dt, ↑ EF, ↑ CO(↑ Pulse Pressure) ↓ MR ↓ LA
Pressure↑ LV Diastolic
Filling↑ RV Stroke
Volume
↓ LVESV ↓ LVEDV
Reverse Remodeling
Cardiac Resynchronization
Yu CM, Circulation ‘02
Cardiac Resynchronization TherapyCardiac Resynchronization Therapy

QoL Overall perception of health
3645
554848
525658
70
Heart Failure NYHA Class IV
Heart Failure NYHA Class III
Heart Failure NYHA Class II
Chronic Bronchitis
Valve disease symptomatic
AF symptomatic
Angina
Depression
General population
Adjusted SF 36 means Hobbs FDR, et al. Eur Heart J 2002
Cardiac Resynchronization TherapyCardiac Resynchronization TherapyQuali sono le ragioni della CRT ?

LBBB
LABB +Incomplete LBBB
NO LBBB
25.2%
67.9.%
6.9%
0
2000
4000
6000
8000
5517
3476
1771
TOTAL POPULATION
NO LBBB
LBBB + LABB +imcomplete LBBB
n°
Prevalence of wide QRS and LBBB in the Study population (N°=5517)
INCHF
Cardiac Resynchronization TherapyCardiac Resynchronization Therapy

Completed 6-MonthCompleted 6-MonthFollow-upFollow-up(n = 201)(n = 201)
Completed 6-MonthCompleted 6-MonthFollow-upFollow-up(n = 215)(n = 215)
16 Death 122 Heart transplant 01 Infection/explant 15 Missed 6M FU 0
Control Control (n = 225)(n = 225)
CRT CRT (n = 228)(n = 228)
Randomized Randomized 6-Month Protocol6-Month Protocol
(n = 453)(n = 453)Enrollment & “Follow Up”
Cardiac Resynchronization TherapyCardiac Resynchronization Therapy
MIRACLE

Submaximal ExerciseDistance Walked in 6 MinutesDistance Walked in 6 Minutes Change from Baseline*Change from Baseline*
00
1010
2020
3030
4040
5050
6060
00 33 66
Follow-up Period (Month)Follow-up Period (Month)
Met
ers
Met
ers
11
P=0.004P=0.004P=0.003P=0.003
P=0.005P=0.005
Baseline (meters)Baseline (meters)291 ± 101
305 ± 85
CRTCRT
ControlControl
Cardiac Resynchronization TherapyCardiac Resynchronization Therapy
MIRACLE
Abraham WT, Fisher WG, Smith AL, et al. N Engl J Med 2002;346:1845-1853

QOL
Cardiac Resynchronization TherapyCardiac Resynchronization Therapy
Change from Baseline*Change from Baseline*
00
55
1010
1515
2020
2525
00 33 66Follow-up Period (Month)Follow-up Period (Month)
Sco
re I
mp
rove
men
t (p
oin
ts)
Sco
re I
mp
rove
men
t (p
oin
ts)
11
P=0.001P=0.001P<0.001P<0.001P<0.001P<0.001
CRTCRT
ControlControl
Minnesota Living with Heart Failure Questionnaire
Baseline (score)Baseline (score)
59 ± 21
59 ± 20
MIRACLE

NYHA Functional Class
00
2020
4040
6060
8080
100100
120120
Nu
mb
er o
f P
atie
nts
Nu
mb
er o
f P
atie
nts
Improved 2 orImproved 2 ormore classesmore classes
Improved 1Improved 1classclass
No ChangeNo Change WorsenedWorsened
ControlControl CRTCRT
6%6%
32%32%
59%59%
4%4%
16%16%
52%52%
30%30%
2%2%
P<0.001P<0.001
Cardiac Resynchronization TherapyCardiac Resynchronization Therapy
MIRACLE
Abraham WT NEJM `02

4 weeks
4 weeks
One Year
4 weeks
Acute Testing at Implant
Randomization Prior to Discharge
Pre-OP Evaluation
Best Unichamber Biventricular
No Pace No Pace
Biventricular Best Unichamber
Best Chronic Pacing Mode
FlexStim
PATH CHF:Study Design PATH CHF
Cardiac Resynchronization TherapyCardiac Resynchronization Therapy

Study DesignPre-dischargePre-discharge
Random-Random-izationization
ControlControl
CRT CRT
CRT CRT Double-Double-BlindBlind
BaselineBaseline SuccessfulSuccessfulImplantImplant
——6 Months—6 Months—
≤≤ 1 week1 week
MIRACLECardiac Resynchronization TherapyCardiac Resynchronization Therapy
• Primary Efficacy NYHA Functional Class Quality of life (Minnesota Living with HF) 6-minute Walk Distance
• Secondary Efficacy Included VO2 peak, Exercise Time, LVEF, LVEDD, MR, QRS Duration, Clinical Composite Response
• Other Protocol Specified Endpoints Death or Worsening Heart Failure (Safety) # Days Spent in Hospital (Health Care Utilization)
OMTOMT

Risk of Sudden Death: Risk of Sudden Death: GISSI-2 TrialGISSI-2 Trial
Patients withoutLV Dysfunction
(LVEF >35%)Maggioni AP. Circulation. 1993;87:312-322.
Patients withLV Dysfunction
(LVEF < 35%)No PVBs1-10 PVBs/h> 10 PVBs/h
0.86
A
0.88
0.90
0.92
0.94
0.96
0.98
1.00
0 30 60 90 120 150 180
Days
Su
rviv
al
p log-rank 0.002
0.88
0.90
0.92
0.94
0.96
0.98
1.00
0 30 60 90 120 150 180
Days
Su
rviv
alB
p log-rank 0.0001
0.86
Cardiac Resynchronization TherapyCardiac Resynchronization Therapy

Baseline ex CPX
ImplantAttempt
SuccessfulImplant
ControlICD
CRTCRT + ICD
Pre-dischargeRandomization
6 Month Follow-up
6 Month Follow-up
CRT
DoubleBlinded
StableMedicalTherapy
≤ 1week
• Class NYHA II• Intent to treat analyses• Comparison between groups• Core labs: metabolic exercise,
echocardiography, and neurohormone data
CRT
Long term follow up every 6 months
CPX
Cardiac Resynchronization TherapyCardiac Resynchronization Therapy
MIRACLE ICD II

210 Class II 429 Class III/IV
98 Completed 6M FU 82 Completed 6M FU
2 Death 2
1 Missed 6M FU 1
101 Control (ICD+OPT) 85 CRT (CRT+ICD+OPT)
639 Enrolled and Implant Attempted
19 Unsuccessful 191 (91%) Successful
186 Randomized
5 not randomized- 1 death- 4 LV lead dislodge.
Cardiac Resynchronization TherapyCardiac Resynchronization Therapy
MIRACLE ICD II

Composite Response
36% 34% 31%
58%
22% 20%
0%
20%
40%
60%
Improved No Change Worsened
Pro
port
ion
Control (n=101) CRT (n=85) Chi-square test
P = 0.01
Cardiac Resynchronization TherapyCardiac Resynchronization Therapy
MIRACLE ICD II

Effect on Ventricular Arrhythmias
• 25/101 pts (Control) 89 VT/VF events
• 18/85 pts (CRT) 61 VT/VF events
25%
21%
0%
5%
10%
15%
20%
25%
Control CRT
p = 0.61During 6 Month Randomization Period
Cardiac Resynchronization TherapyCardiac Resynchronization Therapy
MIRACLE ICD II

79
MADIT II Marzo 2002
Precedenti Linee Guida ACC/AHA per ICDs September 2002
COMPANION Maggio 2004
SCD-HeFT Gennaio 2005
La strada alle nuove linee guida
ESC updated Maggio 2005
ACC/AHA updated Agosto2005
CARE-HF Aprile 2005
Cardiac Resynchronization TherapyCardiac Resynchronization Therapy

80
MADIT II Marzo 2002
Precedenti Linee Guida ACC/AHA per ICDs September 2002
COMPANION Maggio 2004
SCD-HeFT Gennaio 2005
ESC updated Maggio 2005
ACC/AHA updated Agosto2005
CARE-HF Aprile 2005
Cardiac Resynchronization TherapyCardiac Resynchronization Therapy
0
1000
2000
3000
4000
1999 2001 2003 2005
Result s Present ed
Cu
mu
lati
ve
Pa
tie
nts
PATH CHF
MUSTIC SR
MUSTIC AFMIRACLE
CONTAK CD
MIRACLE ICD
PATH CHF II
COMPANION
MIRACLE ICD II
CARE HF
La strada alle nuove linee guida

Hospitalization for HF
Mean Mean ±± SEM SEMN N == 16 16
0
10
20
30
40
da
ys
of
ho
sp
ita
liza
tio
n
1 Year1 YearPre-ImplantPre-Implant
1 Year1 YearPost-ImplantPost-Implant
P P == .003 .003
PATH CHF
Cardiac Resynchronization TherapyCardiac Resynchronization Therapy

MUSTIC Inclusion Criteria (67 pts)
• Dilated cardiomyopathy of any etiology• NYHA Class III (not Class IV) • Optimal individual drug therapy • LBBB and QRS duration >150 msec • Not mentioned AVD• LVEF<35% and LVEDD>60mm• 6-MWT<450m• SR & no conventional PM indication
Cardiac Resynchronization TherapyCardiac Resynchronization Therapy

Composite Response
39%39%34%34%
27%27%
67%67%
17%17% 16%16%
0%0%
20%20%
40%40%
60%60%
ImprovedImproved No ChangeNo Change WorsenedWorsened
Pro
por
tion
Pro
por
tion
Control N=225Control N=225 CRT N=228CRT N=228
Chi-square test
83
363
↓↓ 77%77%
ControlControln=34n=34
CRTCRTn=18n=18
P<0.001P<0.001
Total HF days Hospitalized
Cardiac Resynchronization TherapyCardiac Resynchronization Therapy
MIRACLE

NYHA Class III/IV HF*, NYHA Class III/IV HF*, EF EF ≤≤ 35%, QRS 35%, QRS ≥≥ 130 ms, 130 ms,Stable HF Medical TherapyStable HF Medical Therapy
No indicationNo indicationfor ICDfor ICD
IndicationIndicationfor ICDfor ICD
MIRACLEMIRACLE(InSync)(InSync)
MIRACLE ICDMIRACLE ICD(InSync ICD)(InSync ICD)
* Separate protocol for MIRACLE ICD Class II* Separate protocol for MIRACLE ICD Class II
Inclusion Criteria
MIRACLE ICD trials
W.T. Abraham for MIRACLE and MIRACLE ICD Investigators
Cardiac Resynchronization TherapyCardiac Resynchronization Therapy

BaselineBaseline ImplantImplantAttemptAttempt
SuccessfulSuccessfulImplantImplant
ControlControl CRT CRT
Pre-dischargePre-dischargeRandomizationRandomization
1, 3, 6 1, 3, 6 Month Month
Follow-upFollow-up
1, 3, 6 1, 3, 6 Month Month
Follow-upFollow-up
CRT CRT
DoubleDoubleBlindedBlinded
StableStableMedicalMedicalTherapyTherapy
≤≤ 11weekweek
CRT CRT
Long term follow up Long term follow up every 6 monthsevery 6 months
• 369 randomized patients369 randomized patients• 182 CONTROL and 187 CRT182 CONTROL and 187 CRT• Control: No pacingControl: No pacing• Treatment (CRT): atrial synched pacingTreatment (CRT): atrial synched pacing• OMT for HF stability maintainedOMT for HF stability maintained• ICD active in all patients of MIRACLE ICDICD active in all patients of MIRACLE ICD
MIRACLE ICD study design
W.T. Abraham for MIRACLE and MIRACLE ICD Investigators
Cardiac Resynchronization TherapyCardiac Resynchronization Therapy
182182 187187
369369

Survival
80%
85%
90%
95%
100%
0 1 2 3 4 5 6
Months Since Randomization
% o
f P
atie
nts
Su
rviv
ing
Control n=402 CRT n=415
P=0.42
W.T. Abraham for MIRACLE and MIRACLE ICD Investigators
Cardiac Resynchronization TherapyCardiac Resynchronization TherapyMIRACLE and MIRACLE ICD Trials

Control 225 214 204 197 191 179 70CRT 228 218 213 209 204 201 99
Patients At RiskPatients At Risk
70%70%
75%75%
80%80%
85%85%
90%90%
95%95%
100%100%
00 11 22 33 44 55 66
Months After RandomizationMonths After Randomization
Eve
nt
Fre
eE
ven
t F
ree
Su
rviv
al
Su
rviv
al (
%)
(%
)
CRTCRT
ControlControlP = 0.033P = 0.033Relative risk = 0.60; Relative risk = 0.60; 95% CI (0.37, 0.96)95% CI (0.37, 0.96)
Time to Death or Worsening HF requiring Hospitalization
Cardiac Resynchronization TherapyCardiac Resynchronization Therapy
MIRACLE

Patients selection• Which is the value of QRS within ?
- 30% pts with wide QRS no Mechanic Asinchronism (Yu, Heart ‘03)
- Which cut-off considerate for pts selection ? - Relationship between QRS duration and LV dilation ?
Ventricoli meno dilatati ma con dissincronie regionali
non alterano l’ECG di superficie (durata QRS normale)? (Auricchio A, Yu CM – Heart ‘04)
Cardiac Resynchronization TherapyCardiac Resynchronization Therapy

• Età avanzata• Genesi ischemica della miocardiopatia (controverso)• Assenza di insufficienza valvolare mitralica (Reuter S et a. Am J Cardiol 2002) o IM severa
(Achilli A, Italian Heart J ‘04)• Maggiori volumi telediastolici e telesistolici (Bax JJ, JACC ‘04)• FA permanente - controverso: ablazione NAV?
Speranza di recupero RS con riduz. IM e reverse LV remodeling?
• Classe NYHA IV (?)
Why are the Non-Responders ?Cardiac Resynchronization TherapyCardiac Resynchronization Therapy

E E AA E E AA
Mitral flowMitral flowICTICT IRTIRTETET
Aortic flowAortic flow
ICT+IRT = MPIICT+IRT = MPIETET
InSyncItalianRegistry
LMPI LMPI
RMPI RMPI
1.2 ± 0.671.2 ± 0.67
1.35 ± 0.761.35 ± 0.76
0.8 ± 0.50.8 ± 0.5
0.81 ± 0.390.81 ± 0.39
0.0090.009
0.040.04
Baseline Follow-up p<
Cardiac Resynchronization TherapyCardiac Resynchronization Therapy

Cardiac Resynchronization TherapyCardiac Resynchronization Therapy
Burkhoff D, Am J Phys ‘87
Influence of Pacing-site

Sinusnode
AVnode
Bundlebranch or
diffuse block
Delayed conduction
• Delayed AV sequence
• Mitral regurgitation
• Decreased filling time
Delayed Ventricular ActivationDelayed Ventricular Activation
What is abnormal in the HF pts?What is abnormal in the HF pts?Cardiac Resynchronization TherapyCardiac Resynchronization Therapy

Cardiac Resynchronization TherapyCardiac Resynchronization Therapy
Spragg DD, Circulation ‘03
Regional Alterations in Protein Expression in the Dyssynchronous Failing Heart

VO2
(ml/
min
/mVO
2 (m
l/m
in/m
22 ))
DODO22 (ml/min/m (ml/min/m22))
OO22ERER
Critical DOCritical DO2 2
DISOXIADISOXIA
Critical VOCritical VO22
DODO22 = = QQC C X CaX CaOO22
VOVO22 = = DODO2 2 X X OO22ERER
NormalNormal
DODO22 = =QQC C x (1,34 xx (1,34 x Hb x Sa Hb x SaOO22) x 10) x 10
Cardiac Resynchronization TherapyCardiac Resynchronization Therapy

Physiologic pacing in ICDPhysiologic pacing in ICD
Spragg DD, Circulation ’03
Regional Alterations of Protein Expression
11 CHF-dyssynchronous Interstitial remodelling: fibrosis α-TNF, apoptosis

Cardiac Resynchronization TherapyCardiac Resynchronization Therapy
Burkhoff D, Am J Phys ‘87
Influence of Pacing-site

Blanc et al., Circulation 1997 23 pts mean ± SD
90
100
110
120
130
140
150
SYSTOLIC SYSTOLIC Blood PressureBlood Pressure
RVARVA LV BVRVORVOBASBAS
mm
Hg
mm
Hg
p<.01 p<.03
0
10
20
30
40
Pulmonary Capillary Pulmonary Capillary Wedge PressureWedge Pressure
RVARVA LV BVBVRVORVOBASBAS
p<.01 p<.01
Acute studiesCardiac Resynchronization TherapyCardiac Resynchronization Therapy

Kass, Circulation 99
% C
hang
e%
Cha
nge
RVSRVS LVSLVS
SYSTOLIC PressureSYSTOLIC Pressure
0
2
4
6
8
10
RVSRVS LVSLVS
Max LV Dp/DtMax LV Dp/Dt
0
10
20
30
40
meanmean±±SDSDLBBBRBBB
p<.05p<.05
p<.01p<.01
p<.01p<.01nsns
Acute studiesCardiac Resynchronization TherapyCardiac Resynchronization Therapy

Effects of Ventricular Dyssynchrony on Cardiac Function
Reduced diastolic filling time 1 Weakened contractility 2 Impaired Systolic function (depressed Dp/Dt) Protracted MR 2 Mechanical and temporal dyssynchrony Abnormal septal wall motion Post systolic regional contraction 3
1. Grines CL, et al Circulation 1989 2. Xiao HB, et al Br Heart J 1991 3. Søgaard P, et al. J Am Coll Cardiol 2002
Diminished SV
Cardiac Resynchronization TherapyCardiac Resynchronization Therapy
LVRV

• WHO? Which criteria ?
• WHEN? Which NYHA class ?
• WHERE? RV+LV / LV ?
• WHY? Symptoms / Mortality ?
CRT:CRT: KEY QUESTIONS KEY QUESTIONS
Cardiac Resynchronization TherapyCardiac Resynchronization Therapy

Cardiac Resynchronization TherapyCardiac Resynchronization TherapyWhy the need of CRT ?
Debole Contrazione
AttivazioneSistemi
Neuro-ormonali
Ritenzione idrico-salina
CHF
Attivazione Asincrona

Who are the Non-Responders ?
• STRUMENTALE parametri Eco-TDI-SR, ECO3D (no reverse remodelling)
• CLINICI Sopravvivenza, NYHA class, CHF-H, 6MWT, VO2 etc
• BIPHASIC CURVE
Cardiac Resynchronization TherapyCardiac Resynchronization Therapy

Who are the Non-Responders ?• Improve LVEF less then 25%
(Penicka M, Circulation ’04)• Reduction < 10% LVESV
(Yu CM, Circulation ‘05)• Reduction LVESV index <15%
(Pitzalis MV, JACC ‘02)• Class NYHA invariate or
improvement less then 25% of 6-MWT (Bax et a. JACC 2004)
• Invariate NYHA class or 6MWT, death, CHF-H, No change or improvement < 10% of VO2 peak (Lecoq G, EHJ ’05, MUSTIC, PATH-CHF, COMPANION)
• BNP plasma level, MR entity, HRV, persistence of Inter and Intra-Ventricular Conduction Delay.
Cardiac Resynchronization TherapyCardiac Resynchronization Therapy

Optimization of Pacing VV delayOttimizzare l’intervallo VV comporta un ulteriore incremento della FE anche nei responders (Sogaard, Circulation ‘02)
Il 50% dei paz. mostra beneficio nella preattivazione VS (20-60 msec), il 50% nella preattivazione VD (in acuto) (Porciani, Am J Card ‘05)
Cardiac Resynchronization TherapyCardiac Resynchronization Therapy
(Bordachar P, JACC ‘04)

• Inaccurata selezione dei pazienti sulla base degli indici predittivi
• Presenza di comorbidità elevata
• Stimolazione biventricolare tecnicamente inefficace
• Severe CHF or hemodinamic instability
Why are the Non-Responders ?Cardiac Resynchronization TherapyCardiac Resynchronization Therapy

What does it mean wide QRS ? What does it mean wide QRS ? LBBB more prevalent with Impaired LV
Systolic Function
38%
24%
8%
Moderate/SevereHF (2)
Impaired LVSF(1)
Preserved LVSF(1)
1 Year Survival
11%
16%
QRS <120ms
QRS > 120 ms
P < 0.001
1. Masoudi, et al. JACC ‘032. Aaronson, et al. Circ 97
Cardiac Resynchronization TherapyCardiac Resynchronization Therapy
Long-term (45 Mo) Survival
34%
49%
QRS < 120 ms
QRS > 120 ms
Iuliano et al. AHJ 2002N=669
P < 0.001
Baldasseroni S. EHJ `02 N=5,517

What does it means DYSSYNCHRONYSM ?• VEST study analysis• NYHA Class II – IV pz• 3,654 ECGs digitally
scanned• Age, creatinine, LVEF,
heart rate, and QRS duration found to be independent predictors of mortality
• Relative risk of widest QRS group 5x greater than narrowest
60%
70%
80%
90%
100%
0 60 120 180 240 300 360Days in Trial
Cu
mu
lati
ve S
urv
ival
QRS Duration (msec)
<9090-120
120-170170-220
>220
Adapted from Gottipaty et al. JACC 1999; 33(2):145A (abstract 847-4)
Cardiac Resynchronization TherapyCardiac Resynchronization Therapy

%
Mortality rate in patients with or without LBBB (5517 pts)
0
5
10
15
20
25
301 Year-Mortality
Total Sudden Death
LBBBNo LBBB
Study population
11.9
16.1
10.5
5.5 4.97.3
p<0.001
p<0.001
No LBBBUnadjusted 1
Adjusted 1
RR of Total Death
No LBBB
Unadjusted 1
RR of Sudden Death
Adjusted 1
1.70(1.34-2.21)
1.36(1.15-1.61)
LBBB
1.58(1.21-2.06)
LBBB
1.34(1.05-1.42)
INCHF
Cardiac Resynchronization TherapyCardiac Resynchronization Therapy
LBBB: 25,2%

1 Framingham Heart Study (1948 – 1988) in Atlas of Heart Diseases.2 American Heart Association. Heart Disease and Stroke Statistics—2003 Update.
CHF Patients Survival ResultsCHF Patients Survival Results11
1009080
70
605040
3020100
Prob
abili
ty o
f su
rviv
al, %
Men (Men (n n = 237)= 237)Women (Women (nn = 230) = 230)
Time after CHF diagnosis, years0 2 4 6 8 10
80% of men and 70% of women who have CHF will die within 8
years.2
80% of men and 70% of women who have CHF will die within 8
years.2
Cardiac Resynchronization TherapyCardiac Resynchronization Therapy

Synchronizing the Ventricles: Separation of E- and A- Waves
Surface ECG
IVRT IVRT
A-waveA-wave
Aortic Flow
E-waveE-waveSpectral Doppler
PR PR
LVFTLVFT
Aortic Flow
Cardiac Resynchronization TherapyCardiac Resynchronization Therapy
Karloff, PACE ‘87

Cumulative Enrollment in C.R. Cumulative Enrollment in C.R. Randomized TrialsRandomized Trials
0
1000
2000
3000
4000
1999 2001 2003 2005Result s Present ed
Cum
ulat
ive
Patie
nts
PATH CHF
MUSTIC SR
MUSTIC AFMIRACLE
CONTAK CD
MIRACLE ICD
PATH CHF II
COMPANION
MIRACLE ICD II
CARE HF
• • Actual � ProjectedActual � ProjectedDOUG SMITHDOUG SMITH
Cardiac Resynchronization TherapyCardiac Resynchronization Therapy

Cardiac Resynchronization TherapyCardiac Resynchronization Therapy
Kerchhoffs RC, J CV Electr 03
Influence of Pacing-site in CANINE model

Cardiac Resynchronization TherapyCardiac Resynchronization TherapyInfluence of Pacing-site in CANINE model
Kerchhoffs RC, J CV Electr 03

Ansalone G, GIEC ‘05
Pts with LBBB, after CRT PW-DTI, shows an improvement of
mitralic CO respect E-A interval, with reduction of systolic
velocity peak
Patients selectionCardiac Resynchronization TherapyCardiac Resynchronization Therapy
INTRA-VCD Eco M-mode (validate in QRS wide) PW-TDI Strain Rate Echo 3D

Optimization of Pacing VV delayOttimizzare l’intervallo VV comporta un ulteriore incremento della FE anche nei responders (Sogaard, Circulation ‘02)
Il 50% dei paz. mostra beneficio nella preattivazione VS (20-60 msec), il 50% nella preattivazione VD (in acuto) (Porciani, Am J Card ‘05)
Cardiac Resynchronization TherapyCardiac Resynchronization Therapy
(Bordachar P, JACC ‘04)

laterale (35%) anteriore (26%) posteriore (23%) infero-settale (16%)
(Ansalone, Am Heart J ‘01)
Inferiore (45%)Laterale (30%)Posteriore (25%)Settale (16%)Anterosettale (5%)
(Yu, JACC ‘05)
Optimization of CRTCardiac Resynchronization TherapyCardiac Resynchronization Therapy
I segmenti maggiormente interessati dal ritardo sono:
If the objective of CRT is pacing the more delayed wall, the selection of the site of stimulation will be relevant

Improvement in Peak VOImprovement in Peak VO22
-0.5-0.5
0.00.0
0.50.5
1.01.0
1.51.52.02.0
ControlControl(n=145)(n=145)
CRTCRT(n=158)(n=158)
ml/
kg/m
inm
l/kg
/min
P=0.009P=0.009
Improvement in Improvement in Total Exercise TimeTotal Exercise Time
00
3030
6060
9090
120120
ControlControl(n=146)(n=146)
CRTCRT(n=159)(n=159)
seco
nds
seco
nds
P=0.001P=0.001
Baseline Baseline (ml/kg/min)(ml/kg/min)
13.7 ± 3.8
14.0 ± 3.5
BaselineBaseline (secondsseconds)
462 ± 217
484 ± 209
Metabolic ExerciseMIRACLE
Nelson et al. Circulation ‘00Ukkonen et al. Circulation ‘03
Cardiac Resynchronization TherapyCardiac Resynchronization Therapy

Current treatment of CHFFunctional improvement
Mortality reduction
– pump failure
– sudden death
DrugsDrugsLV/LV/BiVBiV Pacing Pacing ?
ICDICDDrugsDrugs
LV/LV/BiVBiVICD ?ICD ?
≈ 15% of all conventional ICD could be eligible for BVP
Cardiac Resynchronization TherapyCardiac Resynchronization Therapy